Snoring & Sleep Apnea
Signs that you may need to be tested:
- Do you snore?
- Can’t make it through the day without feeling tired or fatigued?
- Become sleepy while driving?
- Can’t get through the night without getting up and going to the bathroom?
- Have High blood pressure, high cholesterol, type 2 diabetes or acid reflux?
- Do you grind your teeth or wake up in the morning with headaches?
If you answered yes to any of these questions, you owe it to yourself to be tested for nighttime breathing disorders which include snoring, Obstructive Sleep Apnea- a narrowed or obstructed airway when an individual tries to breathe while sleeping, or Hypopnea – the drop of oxygen in the blood while sleeping.
Did you know:
- Approximately 40 million Americans suffer from Obstructive Sleep Apnea and of those only 10 percent have been diagnosed.
- Of those diagnosed, only 25 percent can tolerate their current treatment.
- 70 percent of snorers have some level of sleep apnea.
- Severe sleep apnea raises risk of dying early by 46 percent
- Patients with untreated sleep apnea are 12x more likely to be involved in a car accident and the NTSB rates tired driving more dangerous than drunk driving.
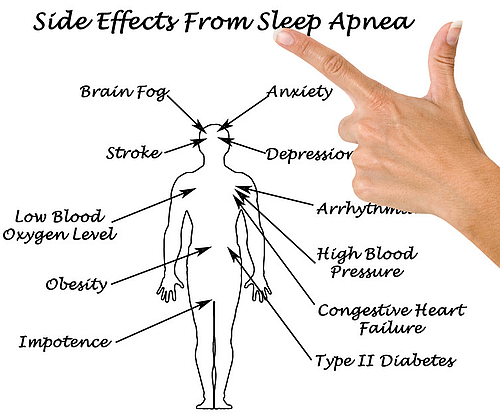
- Sleep apnea his been linked as a contributing factor to:
- High blood pressure
- Coronary artery disease
- Irregular heart rhythms
- Obesity
- What does this mean? A markedly increased chance of a heart attack or stroke.
- Current research even suggests a link between Obstructive Sleep Apnea and an increased risk for developing cancer.
- Treatment for Obstructive Sleep Apnea can add 7-10 years life expectancy.
The good news:
 We now have different options for the diagnosis and treatment of Obstructive Sleep Apnea (OSA).
We now have different options for the diagnosis and treatment of Obstructive Sleep Apnea (OSA).
The most common complaint we get from a patient or their bed partner is snoring. Some patients have been recorded snoring up to 90db or louder! That’s the equivalent of a Boeing 737 coming in for a landing, or standing next to someone using a jackhammer. While it can be loud and disruptive, it can also be an indication of a more serious problem.
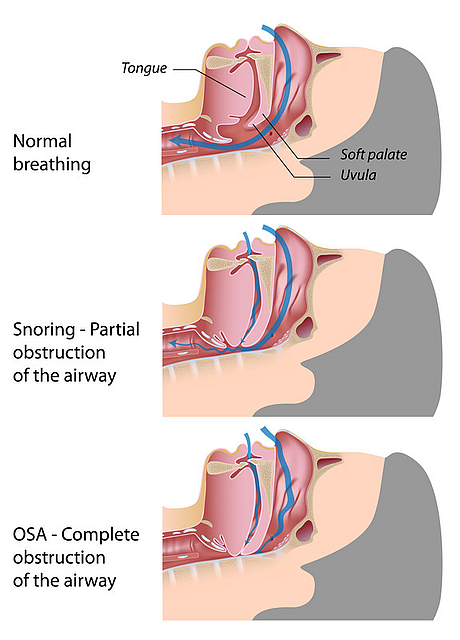
When we fall asleep and start to drift into the deeper stages of sleep, our tissues relax as blood is shunted away from our extremities and towards our core. Our breathing slows and this can allow for tissues in the back of our throat to collapse. Snoring occurs when air passes through the now constricted airway causing those relaxed tissues to vibrate. Loud snoring occurs when that airway is even further restricted. Obstructive Sleep Apnea occurs when the airway gets sealed shut, essentially choking us in our sleep.
Now our bodies are designed to keep us breathing no matter what! When we stop breathing during sleep, our bodies will rouse us from the deeper stages of sleep in order to kick start our breathing apparatus and get air back in our lungs. We may not physically wake up, but we never get into those deep stages of sleep where our bodies repair themselves. So we wake up tired despite sleeping through the night. Our bodies’ starvation of oxygen during the night can lead to cardiovascular issues and type II diabetes. Our bodies’ attempts to push our airway open can lead to grinding our teeth and acid reflux.
The gold standard for treating OSA has been and continues to be the CPAP, a medical device that pumps air into one’s airway creating a balloon like effect so that when the tissues try to relax they are supported by positive air pressure. The problem with a CPAP has always been patient compliance. It’s noisy and uncomfortable and difficult to travel with. There is an alternative. The American Academy of Sleep Medicine recently approved dental sleep appliances as an effective treatment for minor and moderate cases of OSA.
The process begins by filling out a screening form. Dr. Schwab will examine the results of that form and if red flags appear, then we perform a non-invasive examination of your airway and see if there could be signs that you are prone to a full collapse of your airway. If so, a sleep study is ordered. This can be done in one of two ways. We can use a traditional sleep lab, or we have a device in our office that patients can take home and have a sleep study conducted in the comfort of their own home. That information is then examined by a Texas Board Certified Sleep Physician who then renders a diagnosis. If the patient doesn’t have OSA then great! We can make an appliance to help with the snoring. If OSA is present, then Dr. Schwab will discuss the treatment options available based on the Physician’s recommendations.
If a dental device is recommended and accepted, Dr. Schwab will utilize Rhineometry and Pharyngometry to set up the appliance, and after the symptoms of snoring and daytime sleepiness are consistently resolved, a second sleep study will be performed with the appliance to make sure we have adequately decreased the number of OSA events.
If you have questions, or if you have been diagnosed with OSA and would like to discuss alternatives to CPAP, the team at Waco Family Dentistry is here to help!




